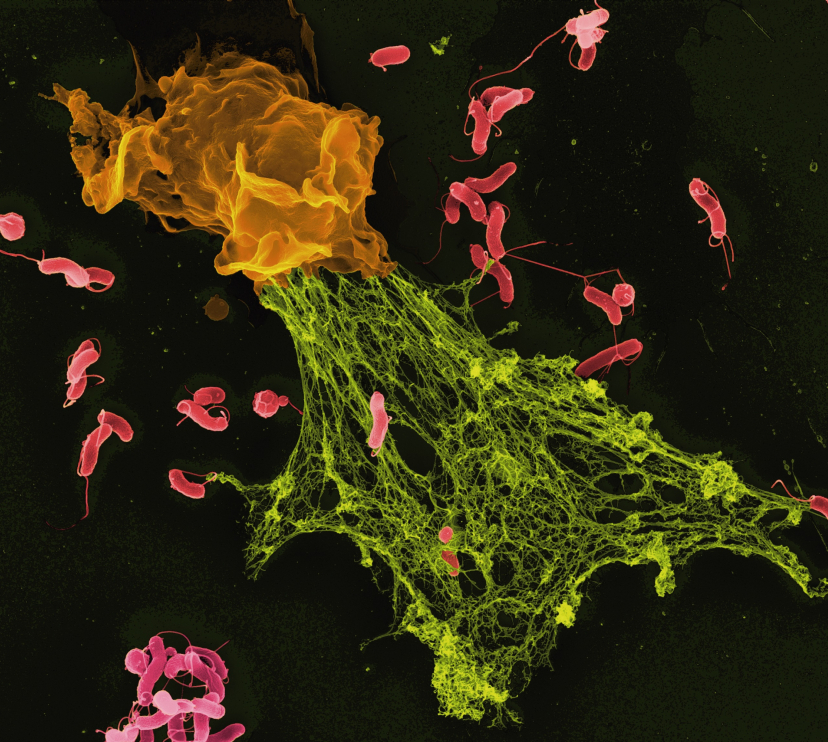
Immunology: the key to understanding the health and medicine of the future
24.04.26
9 minutes readFor decades, immunology occupied a relatively modest place in medical textbooks. Today, however, it has become a central discipline that allows much of human disease to be reinterpreted. Initially studied in relation to infections, we now know that it also plays a fundamental role in the fight against cancer, neurological disorders and a growing number of autoimmune and inflammatory diseases. This cross-cutting perspective underpins the creation of the CaixaResearch Institute, conceived to place the immune system at the centre of research as a common axis of health and disease.
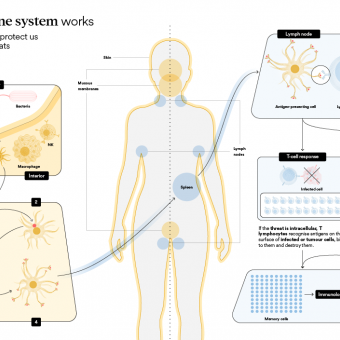
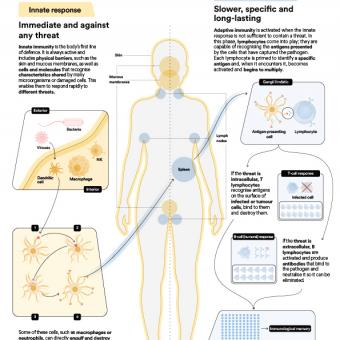
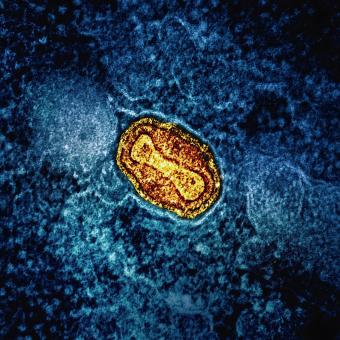
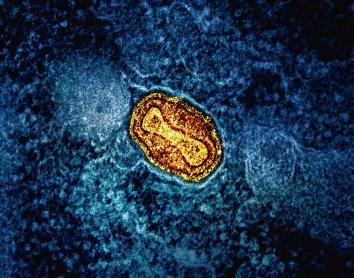
Immunology is a branch of knowledge that studies the immune system and how it functions, analysing how the body identifies its own cells, detects potential external “enemies”, and activates defence mechanisms to keep them under control. Fundamental milestones have been achieved thanks to this knowledge, such as the development of effective vaccines and the eradication of smallpox, one of the greatest achievements of modern medicine.
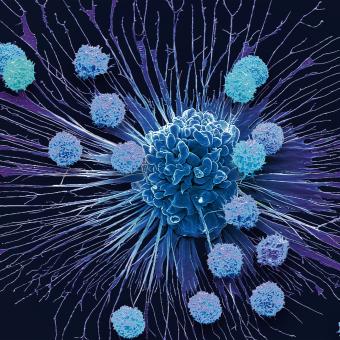
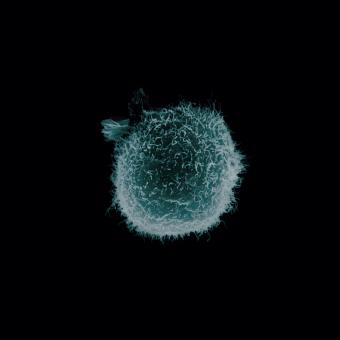
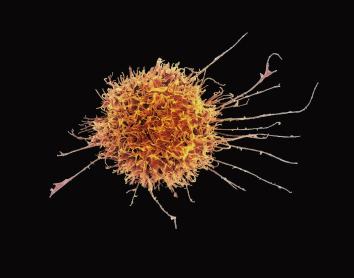
It also studies how this biological machinery protects us from internal threats, such as cancer cells, as well as the sophisticated control mechanisms required to ensure that it stops in time and does not damage our own tissues. More recently, through what is known as immunotherapy, the scientific community is learning to reprogramme immune cells with the aim of modifying the patient’s own cells to act therapeutically.
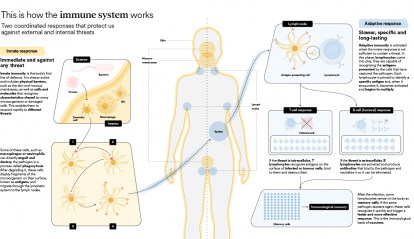
This balance between the external and the internal, between safety and threats, can be compared to a choreography: the immune system must activate whenever something puts us at risk and deactivate once the threat has disappeared. Immunology also studies what happens when one of these steps fails: if the response is insufficient, infections or tumours may progress; if it becomes uncontrolled, the system may react to stimuli that pose no danger or even damage healthy tissues, as occurs in allergies and autoimmune diseases. Understanding the latter, that is, how and why these failures occur, is one of the major challenges of contemporary biomedicine.
The immune system connects virtually all the organs and processes of the body, and its mechanisms influence areas as diverse as infections, brain health, tissue repair, ageing, the development of chronic diseases and, more generally, the body’s overall balance. Deepening our understanding of how it works not only helps explain why we fall ill, but also paves the way for new methods of diagnosing, preventing and treating a wide range of conditions. Immunology is no longer just another discipline; it has become a cross-cutting axis across all branches of medicine and health.
Infections and vaccines: the immune system on
the front line
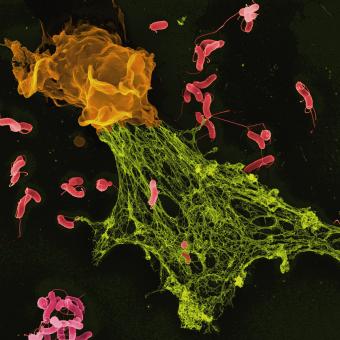
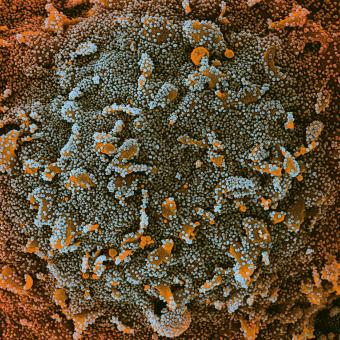
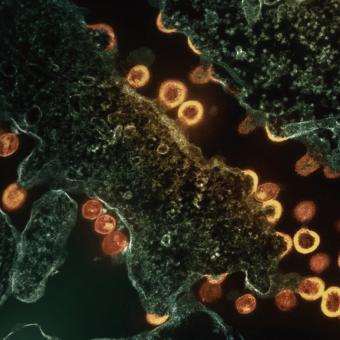
When people think of immunology, the first thing that usually comes to mind is infectious disease. This is no coincidence: since the beginning of human history, the immune system has been essential in confronting external agents such as viruses, bacteria and parasites. And although this remains a central field of immunological research, science is now moving towards increasingly complex questions, driven by new technologies that make it possible to analyse the impact of immunology in many other areas.
From the discovery of the first vaccines to the present day, dozens have been developed and much has been learned about how they work. We now know that not everyone responds in the same way to a given vaccine, nor do people react in the same way to the same infection. This variability, made visible on a global scale during the pandemic, is one of the areas in which immunological research is providing some of the most revealing answers. Understanding these differences is key to designing vaccines that are more effective and equitable, capable of protecting diverse populations. In addition, while some vaccines generate very long-term immunity, others provide more short-lived protection. Understanding why these differences occur is essential for uncovering how long-lasting immune memory is built and for moving towards strategies that avoid the need for repeated booster doses – an issue that science is still working to resolve.
Immunology is also helping to decipher phenomena that until very recently were largely mysterious, such as long COVID or the tolerance developed by certain populations that are continuously exposed to pathogens such as the malaria parasite.
Furthermore, as climate change, population movements and environmental changes favour the spread of emerging viruses, immunological knowledge is becoming an essential tool for anticipating and containing these threats.
When the body’s defences turn inward
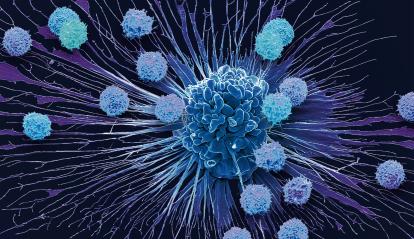
If, in infections, the challenge for the immune system is to recognise and neutralise an external threat, in cancer the challenge is even more complex. In this case, the immune system must detect when cells within the body itself stop functioning properly. Under normal conditions, the immune system identifies these cells displaying abnormal behaviour and destroys them (in a process known as immunosurveillance). However, when these cells learn to evade immune cells, they may begin to proliferate and form tumours.
Understanding how these dynamics arise between the tumour and the immune system has become one of the main priorities of current cancer research.
Another aspect that has become clear is that the immune response always develops within a context in which multiple signals determine whether the system will act effectively or become blocked. It is no longer simply a matter of attacking the tumour, but also of intervening in the system that must recognise it: learning how to modulate the body’s defences, restore their ability to identify the threat, adjust their intensity and direct their action with precision.
Advances in cancer immunotherapy have demonstrated the enormous potential of this approach, but also its limitations. Not everyone responds in the same way to the same treatments, and understanding why remains one of the major unanswered questions. Once again, current research points to the diversity of the immune system and its interaction with particular cellular environments.
The dialogue between the immune system and the
brain
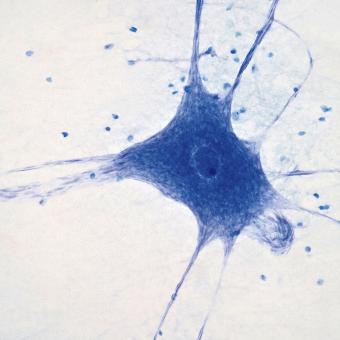
At times, imbalance arises when the immune response is directed towards particularly sensitive areas. For a long time, the brain was considered a territory alien to immunology, protected by an almost impenetrable barrier known as the blood–brain barrier, the brain’s major physical boundary through which immune system cells could not pass. Today, that idea has been left behind.
Neuroimmunology has revealed that certain neurological disorders are driven by poorly regulated immune mechanisms, and identifying these processes has brought about a profound shift. Diseases that were once considered inexplicable or irreversible can now be diagnosed with greater precision and, in many cases, treated. Neuroimmunology has uncovered an entirely new category of diseases in which the immune system is involved, something that, until recently, was not even suspected.
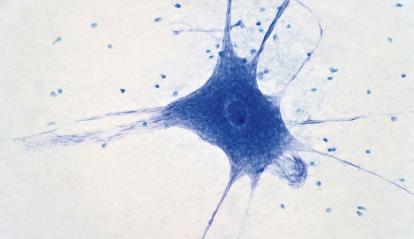
Research in this field has shown that a misdirected immune response can affect essential proteins in the nervous system. Understanding which signals trigger this process allows for better classification of these conditions and intervention before the damage becomes irreversible.
Moreover, this connection between immunity and the brain is broadening the focus to include diseases that have traditionally been studied from other perspectives, such as certain neurodegenerative disorders. Persistent activation of immune mechanisms, the breakdown of regulatory systems, or sustained inflammatory signalling are now emerging as important pieces of a much larger puzzle that is forcing us to rethink the relationship between the brain and the rest of the body.
When we respond to non-existent threats or
against ourselves: autoimmunity and dysregulation
Occasionally, the immune system fails in its mechanisms for distinguishing between what requires a response and what does not. In such cases, it may act aggressively against the body’s own structures, as occurs in autoimmunity, or respond in a disproportionate way to external agents that would not in themselves cause significant harm, as happens in allergies.
Research has shown that multiple factors converge in this process. Genetics explains part of it, but not all. Each person’s immune history, their exposure to previous infections and the way their immune system has learned to respond throughout life all play a decisive role.
Beyond merely relieving symptoms, immunology offers the possibility of intervening in the underlying causes of the problem: restoring regulatory mechanisms, modulating the intensity of the immune response and enabling the system to regain its capacity for self-regulation. This is not a simple task, but it opens the door to more precise and longer-lasting treatments.
A new stage for biomedical research
As immunology has progressively revealed its role in fields as diverse as infections, cancer, neurology and inflammatory diseases, it has become clear that it is not simply another discipline but a central axis that runs through the whole of biomedicine. Understanding how the immune system works – and especially how it loses its balance – makes it possible to connect pieces that for decades were studied separately and to find solutions where there was previously little hope. Today, immunology stands at the meeting point of many of the most significant medical advances.
Diseases linked to the immune system affect hundreds of millions of people worldwide. This new perspective will make it possible to reduce the extremely high mortality associated with infectious diseases, which currently account for between eight and twelve million deaths each year, as well as those attributed to cancer, with approximately ten million annually. It will also help improve quality of life and support the development of new treatments for people with allergic diseases (affecting 30–40% of the population), chronic inflammatory diseases (around five million people) or autoimmune diseases (up to 10% of the population). In addition, it will contribute to developing new approaches to various cardiovascular and neurological diseases that affect more than three billion people and cause around thirty million deaths each year.
The mission of the CaixaResearch Institute lies precisely at this turning point: to promote research that views the immune system as an integrated whole capable of generating fundamental knowledge while also opening new avenues for the prevention, diagnosis and treatment of disease. It is a commitment to science that seeks to gain a profound understanding of the mechanisms of health and disease, and to generate a lasting impact on the wellbeing of society.